iStock
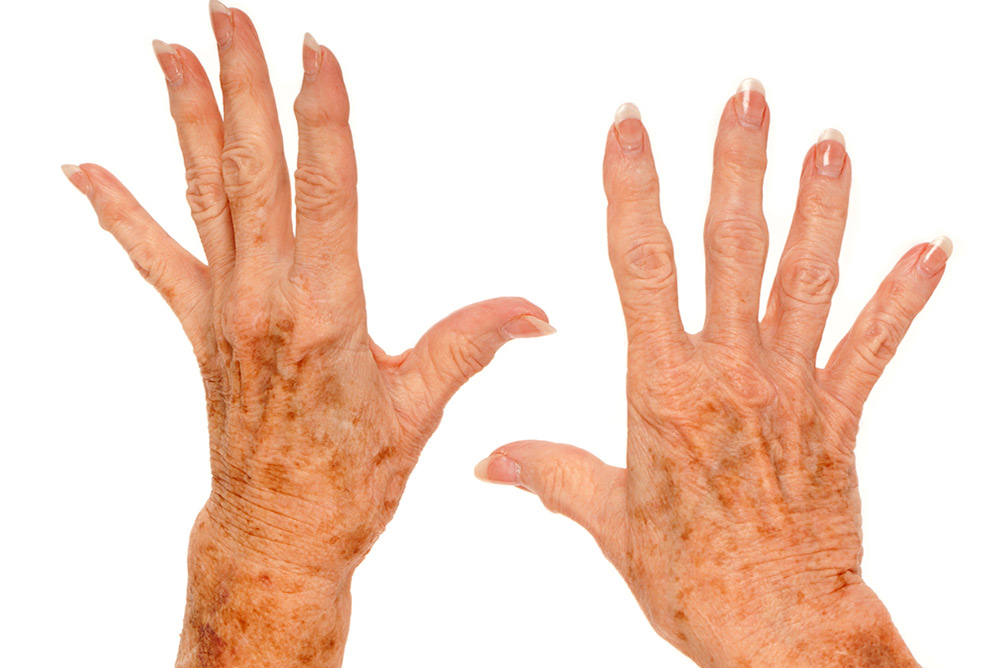
IT’S THAT TIME OF YEAR for inspecting the summer’s sun damage, especially for those who’ve had trouble resisting cool pool waters or unfettered (by lanes and lane hogs) ocean waves.
The villainous rays are ultraviolet radiation A and B, which can alter genetic material in skin cells. The more commonly encountered UVA rays, which cause tanning and wrinkles and contribute to skin cancer, can penetrate clouds and windows, and protection should be applied every day. UVB rays, responsible for intense sunburns and skin cancer, are strongest in the spring and summer, between 10 a.m. and 4 p.m. and at high altitudes. Reflective surfaces like snow and ice can increase the intensity of UVB rays, as can swimming in pools where both the water surface and the pool bottom reflect the rays.
Examining Sun Spots
Before deciding on treatment, pigmented spots must be examined to see whether they have any “substance” in addition to color, writes Scottsdale, Arizona, dermatologist Charles Bollman on Quora.com. Spots with any perceptible thickening might need destructive treatments like liquid nitrogen and electrocautery, and anything suspicious should be biopsied.
Even flat, seemingly innocuous sun spots, called solar lentigos or lentigines, should be checked by a dermatologist, because they are created by a similar proliferation of melanocytes — which produce skin pigment or melanin — as that causing dangerous melanomas. Once sun spots are determined to be non-cancerous, the first treatment is often vitamin C cream or ointment to increase elastin and collagen in the skin for a smoother look. Recommended formulations should come from a dermatologist because many creams are unstable.
If topical vitamin C produces no negative or allergic reactions, a lightening agent containing hydroquinone — usually 2% concentration — can be added. Next come retinoids, vitamin A derivatives that can stimulate the sloughing off of darkened skin cells. Dark sun spots on lighter skinned individuals tend to be more superficial and respond better to topical hydroquinone or retinol. Some dermatologists recommend exfoliants containing glycolic or other acids to stimulate faster skin cell turnover.
Microneedling, IPL
To produce lighter, smoother skin over the entire face, micro-needling — PIN for percutaneous induction therapy or collagen PIN — is done with what looks like a fat pen holding 12 or 36 microneedles to create many tiny injuries that can stimulate collagen and elastin production and also be used to insert vitamin C deeper into the skin. Micro-needling is performed in a series of three to six treatments, usually one month apart — at about $300/treatment, generally not covered by insurance — and is also used for acne and scarring.
Another option, intense pulsed light (IPL), uses multiple wavelengths and is considered non-ablative or not destructive — in contrast to lasers, which deliver only one intense wavelength and are ablative. Some dermatologists recommend using IPL on flat sun spots, usually in more than one treatment, and in conjunction with topical therapies. IPL, which has a slight risk of hyperpigmentation, has other uses including hair removal.
The next, more aggressive step, the ablative treatments, include superficial chemical peels using salicylic acid and glycolic acid, dermabrasion, lasers that remove darkened layers of the epidermal or top layers of skin and can stimulate growth of new skin cells. These treatments carry slight risks of hyper- and hypo-pigmentation as well as burns and scarring; and subsequent sun exposure can cause intense burns.
Skin Cancer
Raised dark spots must be biopsied to determine if they are cancerous. Skin cancer occurs three times more often in men than women; the risk increases with age; and it is more common in people with fair skin: an estimated 40 to 50% of those with fair skin will develop at least one skin cancer by age 65, especially in places with more intense sunshine.
Skin cancers are separated into two groups: non-melanoma and melanoma. Three out of four skin cancers are basal cell carcinomas, which develop from basal cells on the surface of the skin and usually appear as pearly or waxy bumps or flat, flesh-colored or brown scar-like lesions. Basal cell cancers are usually benign and slow-growing but should be removed.
Squamous cell carcinoma, relatively uncommon and more often found in men than women, develops from keratinocytes, skin cells that lie under the top layer of the epidermis, and usually appears as firm red nodules or flat lesions with a scaly surface. When these carcinomas appear as an elevated growth with a central hole, they are called “rat-bite” tumors. Squamous cell carcinomas are likely to be malignant and invasive —spreading to local lymph nodes — and must be removed.
Melanoma, most often caused by a brief intense exposure or blistering sunburn and in those with a family history, can be aggressive and life-threatening. It generally appears first on extremities and often on the chest or the back.
The five symptoms for determining which lesions might be cancerous are known as ABCDE: Asymmetry (not symmetrical); Border (jagged or uneven); Color (more than one); Diameter (larger); and Evolving (changing in color, size and shape).
The one good thing often said about skin cancer is that it is always visible.
— Mary Carpenter
Mary Carpenter is the Well-Being editor of MyLittleBird. Her last post discussed the effect of anger on the heart.
Look for Mary’s story on sunscreens coming later this fall.
