Brieflands.com
By Mary Carpenter
“FIBERS IN a variety of colors protrude out of my skin like mushrooms,” said Joni Mitchell about her Morgellons disease, which made her feel as if she were being “eaten alive.” Mitchell remained housebound following reports of a 2015 brain aneurysm but began performing in public again in 2022, appearing most recently at the 2024 Grammy awards.
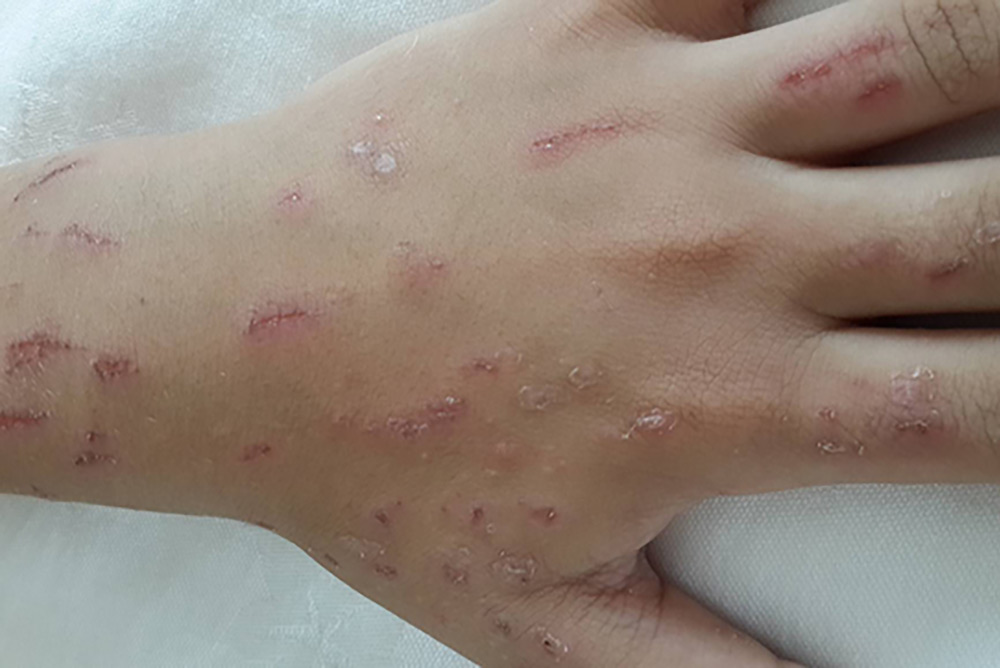
Morgellons disease (MD) is a “disfiguring and distressing condition,” according to dermatology researchers at Wake Forest. Symptoms include sensations of crawling, biting and stinging on the skin that can be very painful; and multiple, non-healing skin wounds. But the existence of red, blue, black and white fibers in the skin is the most notable complaint—hence the nickname “fiber disease.” Patients bring scabs and other skin samples with embedded fibers—called “matchbox” or specimen signs —for testing.
Since the first reported U.S. cases in 2002, the estimated prevalence of Morgellons disease is about 3.6 cases/100,000, most often in white, middle-aged women,” according to a 2012 CDC analysis of 115 patients. The study also determined that the protruding fibers were made of cotton—not bodily substances—and traced the skin sores to “long-term picking and scratching the skin.”
The diagnosis of Morgellons symptoms, based on the study, was “delusional parasitosis,” a psychiatric condition in which sufferers erroneously believe bugs are infesting their skin. (Ekbom Syndrome is a related form of delusional parasitosis.) But lack of general awareness about the condition, even among doctors, can be upsetting for patients—as can receiving an unexpected psychiatric diagnosis for what had looked like a skin disease that can even make symptoms worse.
Multi-system symptoms of Morgellons, on the other hand, are similar to those of Lyme disease (LD)—fatigue, itching, joint aches, loss of short-term memory, difficulty concentrating, insomnia. But after the CDC tested for and eliminated Lyme, Morgellons researchers at Oklahoma State University agreed that “there is no evidence” linking MD to the spirochetes that cause Lyme.
Adding to a fraught history of Lyme disease research, a recent review of literature connecting MD to Lyme found “most of the studies…were published by the same group of authors,” according to Healthline. In addition, the authors “sometimes reuse participants across their studies…one researcher in this group has previously been accused of scientific misconduct.”
But supporters of the MD-Lyme connection point insist that, when employing testing that is “sensitive and specific…Borrelia spirochetes are readily detectable in MD tissue,” write Canadian microbiologist Marianne Middelveen and colleagues. The researchers also contend that MRI imaging shows alterations in gray matter that could be linked to spirochetal infection.
In addition, careful sectioning and staining of skin samples “determine the keratin and collagen nature of these fibers,” the Canadian researchers assert. Linking these fibers to Lyme, they suggest that “underlying spirochetal infection causes a filamentous dermopathy that is accompanied by an array of LD-like multisystem symptoms.”
They also contest the CDC’s link of MD to delusions. In their paper, “History of Morgellons Disease: from delusion to definition,” they say that the CDC conclusions did not meet conditions for the diagnosis of delusional disorder based on the DSM 5 —the diagnostic manual for psychiatric conditions—notably that any possible physical cause must be excluded.
Delusional disorders must involve “false beliefs based on incorrect inference about external reality that persist despite the evidence to the contrary,” according to the DSM 5. The beliefs must last for at least one month with no other psychotic symptoms.
Delusional disorders share overlapping symptoms with other diagnoses—notably the “overvalued ideas” present in OCD, body dysmorphic disorder and hypochondriasis. But while OCD often involves mistaken ideas, for example, about cleanliness, that diagnosis requires repetitive, ritualistic behaviors that are absent in delusional disorders.
Delusions in one sub-category, “somatic” (referring to bodily function or sensation), range from the “bizarre” —such as that one’s bones are twisted around each other; to non-bizarre—which “mirror real health conditions,” such as broken bones. With Morgellons disease, colorful fibers protruding from the skin are bizarre, but the accompanying non-bizarre itching and skin eruptions occur commonly with real skin disorders, such as allergies, dermatitis and parasitic diseases.
Other non-bizarre delusions include partial paralysis, bodily odors and pregnancy. Reported cases include a man who complained that he was unable to sleep at night, despite tests showing he slept for many hours; and a woman who could feel a foreign substance in her mouth that interfered with eating, although no such substance could be found.
Defining MD as a psychiatric condition also gained support because symptoms respond positively to antipsychotic drugs, which target the neurotransmitters dopamine and serotonin. On the other hand, “reduced growth of parasites and anti-pruritic properties” are listed as off-label effects of these medications, according to Middelveen.
Treatment for Morgellons often includes psychological approaches, such as cognitive behavior therapy. But because the belief of MD sufferers that they have a physical disease is so difficult to dislodge, many are resistant to or upset by such recommendations.
Another confounding issue: one cause of delusional parasitosis is recreational drug use—with “coke bugs” and “meth mites.” In a study of 147 patients complaining of bug infestation, 11% had a history of drug use (methamphetamines, cocaine, heroin, marijuana and other street drugs), according to Middelveen.
Among MD sufferers, Joni Mitchell has admitted to “taking a lot of drugs over the years, including mounds of coke,” according to the Daily Mail. But she was also a victim of childhood polio, a potential infectious link for MD that has not yet been pursued.
—Mary Carpenter regularly reports on topical subjects in health and medicine.

I echo Cynthia’s comment. Though I did know about Joni Mitchell, I really didn’t know what the disease was. Leave it to male doctors and researchers to say it’s all in your head. Very informative piece.
Mary,
Thank you! This was fascinating…! I had no idea that Joni Mitchell suffered from such a strange and debilitating condition. Unfortunately, it’s typical of the medical establishment to label a confounding disease that affects primarily women ‘hysteria’, when they are unable to discover cause.
Great job!
Cindy