iStock
“Our clothing was insufficient to protect us from the severe cold: we had no boots, the snow got into our shoes and melted there: our ungloved hands became numbed and covered with chilblains, as were our feet…” at Lowood, the charity school for orphans in Jane Eyre.
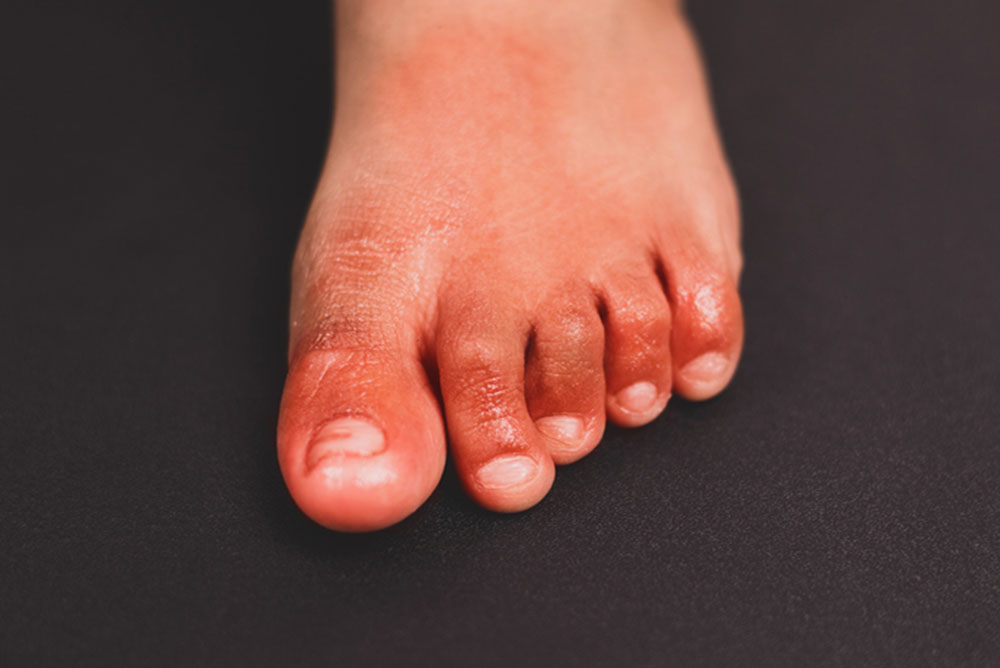
WHEN PHILADELPHIA Charlotte Bronté aficionado L.N. noticed purple spots on the tips of two toes that had been hurting, her first reaction was embarrassment at having the“antique ailment” chilblains, which occur primarily on the hands and feet. The purplish or bluish-red color distinguishes chilblains, also called pernio, from other reactions to cold.
Also described as a “pernio-like reaction, “Covid toes” most often appear in young adults and children—while the most common skin sign of Covid-19 infection is a measles-like rash. Like chilblains, the purplish bumps of Covid toes can arise without any sensation or can cause itching, blisters or pain.
Chilblains—occurring when tiny blood vessels in the fingers and toes swell or leak blood—happen in weather that is cold but not freezing; in temperatures as high as 60 degrees F.; most often in damp cold and regions with high humidity; and usually after repeated exposure. Chilblains most often last two to three weeks, although in England’s damp, cold winters, chilblains are common and can last for several months.
By contrast, frostbite occurs in below-freezing temperatures and freezes the skin and tissues beneath the skin. Along with Raynaud’s disease, frostbite causes skin to look pale or bluish; while cold urticaria and cellulitis make the skin turn abnormally red. Itching and red patches can accompany all of these conditions.
(How cold air feels on your skin and how much heat is lost from the body depend on the so-called “feels-like” temperature—feels-like 25 degrees can cause frostbite even when air temperature is above 32, which takes into account both humidity and the wind speed at around five feet. At lower temperatures, wind speed is more important because it strips the thin layer of warm air above the skin; while at higher temperatures, humidity has the greater impact because it impedes perspiration that helps release body heat.)
“No one knows exactly what causes chilblains,” according to the Mayo Clinic. The tiny blood vessels may swell and become inflamed in response to the cold. Alternatively, rewarming causes the “small vessels to expand more quickly than nearby larger blood vessels can handle…results in a bottleneck effect and blood leaking into nearby tissues.”
In rewarming too quickly—with strenuous rubbing or hot water or air—blood vessels that have narrowed with cold can’t handle the sudden increased blood flow that accompanies warmth. Reheating should instead occur gradually “with warm (not hot) water and without rubbing or slapping.”
The swelling that results when blood leaks into tissue can irritate the nerves and cause pain, which “may represent an allergic reaction or hypersensitivity to the cold.” Additional causes of chilblains include circulatory or cardiovascular diseases, genetic factors, hormonal changes and autoimmune diseases, such as lupus. Perniosis occurs more often in females, and more often in women who are very thin.
For some, perniosis is a seasonal inflammatory disorder but can last for years if untreated and exposure to damp cold persists. Lotions and moisturizers ease most symptoms, and steroid creams help with itching and swelling. Blisters caused by chilblains will heal faster when kept clean, warm and dry, but any sign of infection requires a doctor’s visit.
Tight-fitting clothing may increase susceptibility to chilblains in cold weather by restricting blood flow, which causes a decrease in skin temperature in those areas. Perniosis of the thighs “more commonly affects young females who wear tight-fitting pants,” according to the National Organization for Rare Disorders. “It is characterized by red or bluish patches on the…upper hip region and on the outside of the thighs.”
For those with persistent swelling in the lower limbs, compression socks or stockings can help reduce extra fluid, which will in turn improve the skin’s ability to receive optimal amounts of oxygen. Compression can be especially important for wound healing—but is not advised in cases of impaired sensitivity in the feet and legs.
Keeping skin healthy to avoid adverse reactions to the cold can involve maintaining pH levels just below 5, because skin is “weakly acidic”—while most adults average closer to 5.7. Keeping pH low can also help with dry skin, and acidic cleansers can help combat acne.
Healthy skin may also benefit from bathing less often, according to Atlantic staff writer and Yale School of Public Health lecturer James Hamblin. Says Hamblin, “Bathing disrupts our skin’s microbiome, which has particular importance as our initial defense against pathogens. Maintaining microbiome health can help prevent outbreaks of acne, eczema and psoriasis—which can involve “an interplay between your immune system and the microbes on your skin.”
Hamblin believes that overcleansing may also interfere with skin signals of underlying health problems. As of September, 2020, Hamblin had gone five years without a shower—described in his book Clean: The New Science of Skin. Although he maintains hygiene by frequent hand-washing, people have called him “gross.”
Skin health care may be especially important for feet, which benefit from regular inspection and moisturizing. I have tried to do this more vigilantly since getting advice from my ex-mother-in-law, though I ignored it at first. With age, feet need better care.
—Mary Carpenter
Mary Carpenter regularly reports on topical issues in health and medicine.

Very helpful. I have lots of questions for my primary. What is the most common pain treatment used for Pernio/secondary Raynaud’s phenomenon after the blisters and open soars that follow?