 iStock
iStock
EVEN AS uses—from bladder issues to severe underarm sweating (hyperhidrosis)—for Botox (botulinum toxin) treatments grow, women looking for a “more natural” approach are turning to platelet-rich plasma (PRP) therapy for some of the same conditions and for hair loss.
In 2014, seven million people sought treatment with Botox, the most common cosmetic procedure performed today. In the wild, infection with Clostridium botulinum causes botulism, which starts by paralyzing the muscles of the face, mouth, and throat, spreads to the rest of the body, and, when it affects the diaphragm muscles, causes death—with outbreaks as recently as May, 2017, in California.
Along with plumping facial lines and wrinkles, Botox injections can elevate the eyebrows; treat eye spasms or twitches (blepharospasm); and help relieve neck contracture, spasticity, migraines and chronic pain. Using Botox to smooth the glabella—the skin between the eyebrows that wrinkles with frowning —has aided in treatment of depression.
Botox injected into the affected organ—the salivary glands for excess drooling; the skin for sweating—blocks the release of acetylcholine necessary for muscle activity and can also interfere with mediators of pain and inflammation.
For “urgency urinary incontinency,” related to overactivity of the detrusor, the bladder wall muscle, Botox has proved more successful than the primary alternative, an implanted nerve-stimulation device called InterStim. So-called “urge incontinence” affects 17% of women over age 45 and 25% of women over 75.
In a Duke University study of 364 women followed for six months after receiving Botox injections into the bladder wall, daily episodes decreased by 3.9 in those receiving botulinum toxin versus 3.3 for neuromodulation, although the Botox group had three times the rate of urinary tract infections, and some required intermittent self-catheterization.
Most side effects of Botox occur close to the injection site, such as excessive shutting down of muscles when treating bladder problems as well as overactive sweating and drooling; and headaches when treating migraines and smoothing facial lines.
As a “more natural treatment,” the growing popularity of PRP–first used in orthopedics on painful joints—for aging facial skin is part of a larger medical trend of activating boosters from the patient’s own body, New York City plastic surgeon Robert Silich told The New York Post. Another example is stimulating patients’ immune systems to fight some cancers.
For PRP, a centrifuge spins the patient’s blood to separate out plasma containing a high concentration of platelets. With two means of transferring PRP to the skin —microneedling and injection —the FDA’s classification of PRP as a medical device has less exacting standards than those for new drugs.
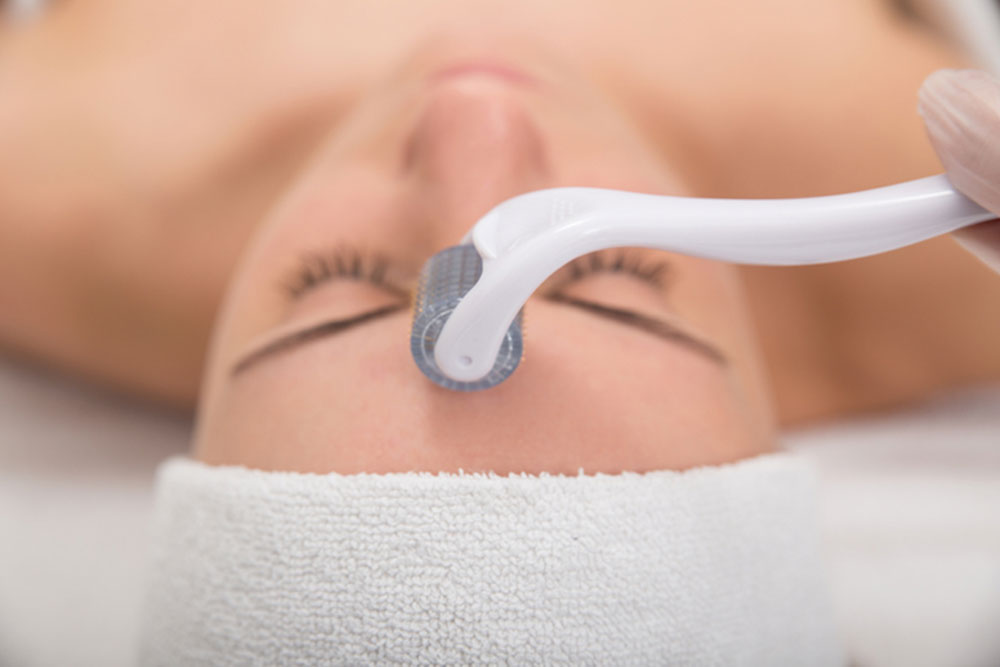
The microneedling used in the “vampire facial” works by way of a cylinder (it looks like a lint roller), covered with tiny needles, which creates many tiny wounds that are subsequently soothed by applications of PRP. The skin can also be plumped with filler. The collagen production stimulated by PRP may produce longer-lasting effects than Botox treatment.
With PRP, there is no chance of an allergic reaction because the injections come from [patients’] own blood,” notes New York dermatologist Marina Peredo.
For hair growth, Peredo says, “This is the first procedure…that has dramatic results and doesn’t need daily upkeep.” In theory, PRP injections trigger and maintain growth by increasing blood supply to the hair follicles, though there is little scientific evidence documenting these effects.
Research support for facial treatment using PRP is also limited. Of 31 patients receiving PRP injections in a multi-center study, only one reported improvement on the Wrinkle Severity Rating Scale (WSRS) while 14 recorded positive results on the Global Aesthetic Improvement Scale (GAIS), though the FACE-Q (measuring satisfaction and quality of life) showed statistically significant increases.
Besides seeming more natural, PRP appeals to vegans because animal testing is not required. But treatment, which costs from $1,500 to $3,500 and requires a series of three injections four to six weeks apart, with boosters every four to six months, is not yet covered by insurance.
Unanswered questions about PRP include the possibility of long-term side-effects as well as how it works for some but not all patients; how many treatments provide the best results; and how much and where to inject PRP. According to the study report: “the quality of evidence supporting its use is poor due to the lack of consistent methods of is preparation and application.”
—Mary Carpenter
Every Tuesday, well-being editor Mary Carpenter reports on health news you can use.
