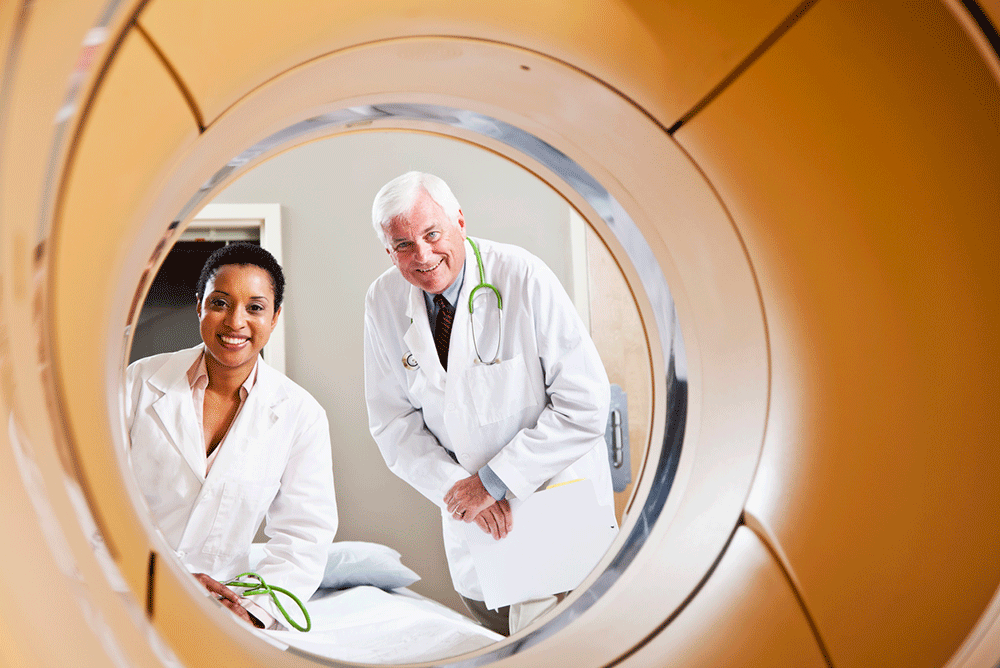
iStock
AFTER YEARS of counting myself among the “worried well”— those who believe their memory is slipping despite high scores on cognitive tests — I enrolled in a clinical trial. The potential upside: a PET (Positron Emission Tomography) scan at no charge, versus the out of-pocket cost of about $3,000.
PET scans can detect amyloid plaque, one of two signature physical changes in the brain linked to Alzheimer’s Disease (AD) that until recently have been observable only after death. Amyloid plaque is suspected of damaging and killing brain cells long before clinical signs of dementia associated with AD appear.
My goal in signing up for the “A4” (Anti-Amyloid Treatment in Asymptomatic Alzheimer’s Disease) study: to have experts monitoring and measuring over several years so I could relax.
Among potential downsides of the trial, however, the worst was that the PET scan could document early signs of AD, thereby moving me to the “worried less-well” category. Another negative: a probably painful spinal tap to examine cerebrospinal fluid (CSF) — optional, but I’d said yes in the interest of acquiring the full battery.
Also distasteful but mandatory: monthly injections of either saline solution (for the control group) or a drug that risked unpleasant side effects and had already failed several trials of efficacy. Because several such drugs targeting amyloid plaque have failed to alter the course of AD in large trials, some experts worry that amyloid appearing on a PET scan has been accumulating for decades, meaning it’s too late for effective treatment and thus for the usefulness of these scans.
A final drawback to the A4: required trips to Georgetown Hospital — good coffee, horrendous parking —starting with four “screening” visits. The first one lasted four hours and, worse, required the presence of an incredibly good-hearted friend, who would provide feedback on my cognitive function for the study’s duration. Post-screening would include more than ten visits, lasting four to five hours each over several years, hopefully without imposing each time on my friend.
Screening visit #2 was the PET scan. Different from CAT scans and MRIs that provide “structural imaging” to determine the size and shape of organs and bones, PET scans provide “functional” images to measure such bodily functions as blood flow, oxygen use and sugar metabolism. PET scans are also categorized as “molecular imaging” because they employ a radioactive tracer. For AD evaluations, the tracer binds to beta-amyloid in the brain, creating “bright” or “hot” spots where large amounts of tracer accumulate.
For my PET, I lay in a darkened room on a narrow platform and am told not to budge. As the radiotracer was injected into my arm, the scanner moved over me and I fell asleep for about half an hour. Not until visit #3 a few weeks later did I learn the results: my PET scan was “clear” of plaques. I was kicked out of the study, ecstatic — at least for now.
AD has traditionally been diagnosed based on cognitive tests like the MMSE (Mini-Mental Status Examination) — the ones I still ace, more or less. But doing poorly on these can indicate that severe damage to the brain has already occurred.
Medical centers such as the University of California at San Francisco (UCSF) have “offered Alzheimer’s disease assessment with amyloid PET scanning for patients with memory complaints” since 2003. According to the UCSF website, “Amyloid PET imaging represents a potential major advance in the assessment of those with cognitive impairment.”
PET scan evidence of early amyloid plaque formation or changes in beta-amyloid levels is most useful to confirm or disprove the AD diagnosis for patients with mild cognitive impairment — rather than for those who have been clearly diagnosed. Questions about the scans persist, however, because many people whose autopsies showed amyloid plaques had exhibited no symptoms of cognitive decline. Clinical studies are now underway to assess the value of PET scans in diagnosing early AD — and confirmation would encourage insurers to cover the scans.
Besides amyloid plaque, the other signature sign of AD is “neurofibrillary tangles” composed of tau proteins that have been tangled and twisted, which impairs their ability to support synaptic connections. Although higher levels of tau protein are present in almost every aging brain, it’s the spreading of tau, for example, into the neocortex, that is associated with serious declines in global cognitive function.
Spreading tau has also been linked to the presence of amyloid plaques in the brain. Many experts believe that “the accumulation of amyloid serves as the kindling for other events” that set off early AD, as Dr. Eric Reiman of the Phoenix-based Banner Alzheimer’s Institute told the New York Times.
“Amyloid may somehow facilitate the spread of tau, or tau may initiate the deposition of amyloid,” explains Berkeley researcher William Jagust. “We don’t know…when amyloid starts to show up, we start to see tau in other parts of the brain [which] may be the beginning of symptomatic Alzheimer’s disease.”
Another area of concern: “brain cells affected by dementia consume less energy than normal brain cells” — which over time can decrease overall brain volume or change the density in affected parts of the brain — according to the Society for Nuclear Medicine and Molecular Imaging (SNMMI) website. “Molecular imaging excels at detecting the cellular changes…often well before structural changes can be seen on CT and MR images.”
Some believe that diagnosis of early Alzheimer’s improves considerably when changes detected by PET scans are combined with elevations in beta-amyloid and tau proteins detected in the cerebrospinal fluid. The hope is that molecular imaging may eventually help monitor disease progression and assess potential treatments.
Meanwhile, “Dramatic Decline in Dementia” was a recent banner headline on the respected medical website STAT, announcing a study of more than 10,500 adults age 65 or older that showed the percentage with dementia, including Alzheimer’s Disease, declined from 11.6% in 2000 to 8.8 percent in 2012.
Increased education among the 2012 group may be the most important explanation, according to University of Michigan researchers. Education “can produce greater cognitive reserve, in which people have enough backup synapses and neurons that losing some to Alzheimer’s still leaves them short of dementia,” Sharon Begley explains in the STAT article. The longitudinal Framingham study also recently produced evidence of the falling risk of dementia among older adults — by about 20% every decade between 1977 and 20008.
If, as currently believed, studying foreign languages and playing musical instruments are the best ways to forestall dementia, there’s a lot more to be done than worrying or spending a sleepy half-hour in a PET scan machine.
— Mary Carpenter
Well-Being editor Mary Carpenter recently posted on the success of non-AA rehab. See more well-being stories.

So glad you were kicked out of the study! Hooray !