iStock
ALTHOUGH IT offers hope for treatment-resistant depression, the first experience of Transcranial Magnetic Stimulation (TMS) for D.C. personal trainer L.M. was so unpleasant that he never returned. As for Electrical Muscle Stimulation (EMS), the advantages of muscle building may be more than offset by workouts that feel like double the usual slog—even if joints are spared.
Stimulators for brain and body are popping up everywhere: those for the body offer muscle building and pain reduction, while options for the brain promise a host of benefits from treating depression and addiction to enhancing cognitive abilities in healthy adults and in those experiencing early dementia.
Such stimulators get their power from either electricity or electromagnetism. For the body, the two options for neuromodulation—that is, altering nerve function—are electrical. For building muscle, EMS targets motor nerves to cause rapid muscle contractions that feel like twitches and spasms.
While the most significant gains occur for post-op patients dealing with muscle atrophy, EMS can enhance muscle size and strength for anyone, including trained athletes—with less stress on joints and tendons. At physical therapy or the gym, clients run or bike on machines, lift weights and perform exercises like squats with electrodes attached to their limbs. While some complain of unpleasant vibrating or burning sensations, Florida lawyer L.K. said using EMS removed ripples from her thighs, leaving them smoothly muscled.
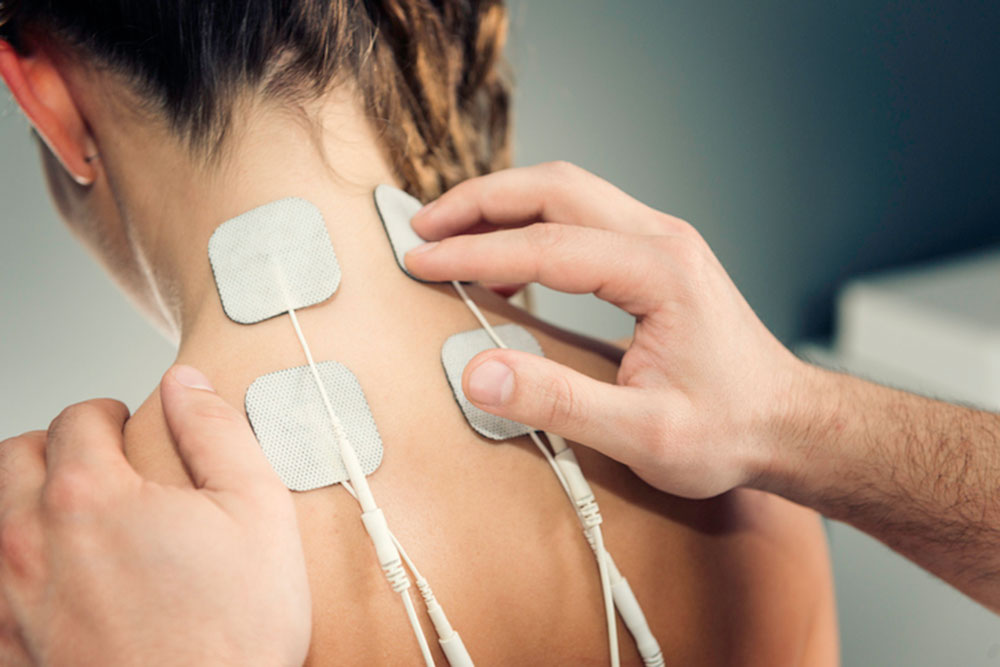
The other body stimulator is Transcutaneous Electrical Nerve Stimulation (TENS), which uses electrodes placed close to areas of pain to create uncomfortable vibrations that interrupt—and thus distract from—pain signals. Based on the gate theory of pain, TENS “provides a competing stimulus,” explains New York City physical therapist C. Shante Cofield. Although TENS helps with symptoms, Cofield warns, “a distraction is not a cure.”
For the brain, the most commonly used neuromodulator is TMS, most often given to those with severe, treatment-resistant depression. Large magnetic coils positioned above the scalp change polarity to produce short magnetic pulses that in turn create an electric current in nearby neurons.
For rTMS —r for repetitive—the coils change polarity at a rapidly increased speed to produce longer-lasting changes in the brain. Patients must remain immobile throughout the half hour or so of treatment —usually five days/week for four to six weeks. Current research aims to understand whether rTMS works better alone or with antidepressants.
But L.M., who stopped after one session, described the sensation as unbearably loud, hard knocking on the skull every three seconds —“painful scalp sensations” that occur for about one-third of patients.
Another treatment for recalcitrant depression—which has also enhanced working memory in healthy adults—is Transcranial Direct Current Stimulation (tDCS). With two electrodes placed directly on the scalp, tDCS can reach deeper areas in the brain than TMS.
The exact positioning of the electrodes, called the montage, depends on treatment goals. For depression, the best montage places one electrode on the left temple and the other above the right eye. Pulses from tDCS modulate the varying cortical excitability that commonly affects those suffering major depression disorder.
In the past decade tDCS treatment has exploded —with 650 studies in 2016—used also for chronic pain, addiction, schizophrenia and epilepsy. In a Chinese study of healthy college students, tDCS in conjunction with cognitive training improved working memory for specific tasks, and that improvement was transferrable to similar untrained working-memory tasks.
In an analysis of 12 studies on dementia patients, tDCS improved memory for a short period; and in one study, had a positive improvement on both memory and language. Personal brain stimulation devices make it possible to do tDCS at home.
(Other electrical options for the brain are more invasive and reserved for severe conditions: Deep Brain Stimulation (DBS), which requires surgery, is a last resort treatment, for example, for Parkinson’s Disease; and ECT, for Electroconvulsive Shock Treatment, requires anesthesia and risks short-term memory loss, and is most given for intractable depression.)
Finally, a new electromagnetic brain option, Transcranial Electromagnetic Treatment (TEMT), appears to directly affect the Alzheimer’s Disease (AD) process by breaking up aggregates of two toxic proteins, A-beta and tau. A TEMT device worn at home enhanced cognitive performance—that is, reversed deficits —in seven of eight patients with mild to moderate AD after two months of twice-daily treatment.
These patients showed changes in AD markers in the blood and spinal fluid, as well as improvements in MRI images of their brains. They had such positive experiences that they asked to keep their devices and remained in an extension study for an average of 17 months.
Because even TENS used for chronic pain can be unpleasant enough to discourage repeated use, the best motivation for using brain and body stimulators may be debilitating issues like dementia or long-lasting depression, or serious muscle atrophy—although smooth thighs are tempting.
—Mary Carpenter
Every Tuesday, well-being editor Mary Carpenter reports on health news you can use.
